The impact of the coronavirus pandemic could present the biggest threat to people’s mental health since the Second World War, according to one of the country’s leading psychiatrists.
Dr Adrian James, the president of the Royal College of Psychiatrists, said that even once the virus was under control, the long-term effect of Covid-19 would have “profound” consequences for people.
He told The Guardian the combined effect of the economic fallout of the virus, the death of loved ones, social consequences of lockdown, and fear of the disease has created a perfect storm in terms of mental ill-health that could continue for a number of years.
“It is probably the biggest hit to mental health since the Second World War,” he said.
”It doesn’t stop when the virus is under control and there are few people in hospital.
“You’ve got to fund the long-term consequences,” he said.
Millions in need of mental health support

According to an analysis conducted by the Centre for Mental Health in October, up to 10 million people in England may require support for depression, anxiety, post-traumatic stress disorders and other mental health difficulties as a result of the pandemic.
This equates to 20 per cent of all adults and 15 per cent of all children.
The study found that around 1.3 million people who have not had mental health problems before are expected to need treatment for moderate to severe anxiety, and 1.8 million treatment for moderate to severe depression.

The charity has called on the Government and NHS to prepare now to meet an increased need for mental health support in the coming months and years.
Data from NHS Digital shows an increased demand for mental health support, with some hospital trusts reporting that their mental health wards have reached capacity.
“The whole system is clearly under pressure,” Dr James said.
Mental health challenges for ‘long Covid’ sufferers
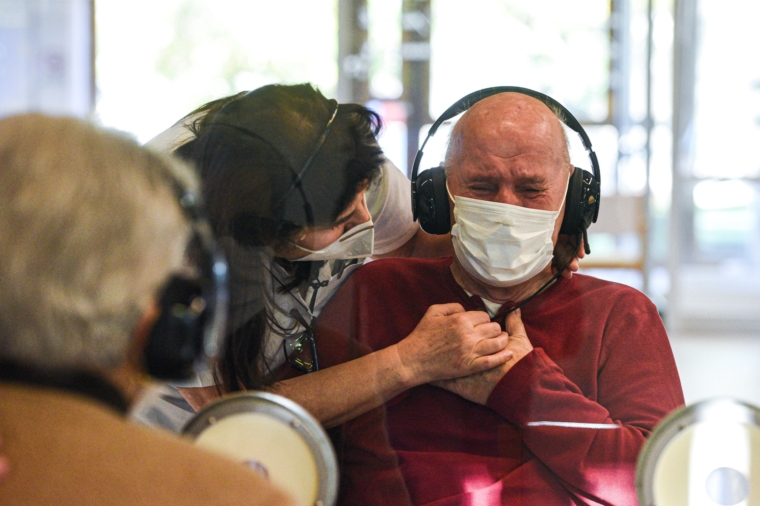
In addition to those who have suffered severe responses to the disease, many people are grieving the loss of loved ones, many of whom were unable to say goodbye in person. Dr James added that the potential for mental health problems emerging in people with “long Covid” is also a concern.
Mass vaccination will not mean an end to mental health challenges, he added, with many requiring additional support to recover.

“It’s very easy to think that when it’s safe to do so, we’ll all be out and about again straight away, but I think it’s going to take a while to get people used to that,” he said.
“The people most likely to suffer are older adults who have got used to self-isolating.”
He added: “We’ll need to support the voluntary sector, the charities, that help them get out of the house to socialise and engage in meaningful activities. We know that when you get older, if you lose your connections for a bit, you can give up on them.”
‘Mental health emergency’
Before Christmas, mental health charity Mind said that the UK was experiencing a “mental health emergency”.
In November, it said that more people had experienced a mental health crisis during the pandemic than ever before.
Paul Farmer, Chief Executive of Mind, told i that while it was “too early” to assess the long-term impact of the pandemic on the nation’s health, it was clear more people were struggling because of it.
He said: “Some of us are experiencing mental health problems for the first time and people with existing mental health problems are finding they are getting worse.”
Mr Farmer noted that early intervention was crucial.
“The earlier people receive support for their mental health, the more likely they are to benefit from treatment.
“As we enter tighter restrictions and possibly another national lockdown it’s crucial well-resourced, timely mental health treatment must be available for those who need it.

“Services must continue to adapt to make sure nobody falls through the gaps, such as offering digital or over the phone support, if face-to-face services close again.”
He added that the NHS had “a responsibility” to communicate how people can access help “before people become more unwell, reach crisis point, and people stop being able to get the support they need.
“The UK Government has recognised the need to protect face to face mental health services, with their winter plan showing that the responsibility for mental health does not just lie with Department for Health and Social Care or the NHS.
“That’s why the next step should be a cross-governmental plan, as soon as possible, that covers all aspects of people’s lives and recognises the role every department must play in dealing with the long-term mental health impacts of coronavirus,” he said.
Six tips for positive mental health this winter
Keep active: Even if it’s a daily walk to the corner shop and back, getting the blood pumping around your body can increase ‘happy’ chemicals in the brain, such as serotonin
Lighten up: Exposure to natural daylight helps our bodies product vitamin D, improves our mood, sleeping patterns and productivity. If you can’t get outside, consider investing in a light box, which shares some of the benefits of natural light
Start a new hobby: Whether it’s trying a new recipe, learning to knit, or starting a new book, set yourself a small goal to focus your energy
Meditate: Meditation can reduce anxiety and stress, help you sleep better and improve relationships
Make time to talk: While we might not be able to see people in person, staying in touch with loved ones is vital for wellbeing, whether it’s a weekly phone call or a daily text message
Eat healthily: Sweets, sugary snacks and alcohol can see sugar levels peak and drop, leaving you feeling tired, irritated and depressed. Eating a diet full of fruit and vegetables helps maintain blood sugar levels by releasing energy slowly throughout your body
If you are experiencing feelings of distress and isolation, or are struggling to cope, The Samaritans offers support 24 hours a day, seven days a week. You can speak to someone for free over the phone, in confidence, on 116 123 (UK and ROI), email jo@samaritans.org, or visit the Samaritans website to find details of your nearest branch.

